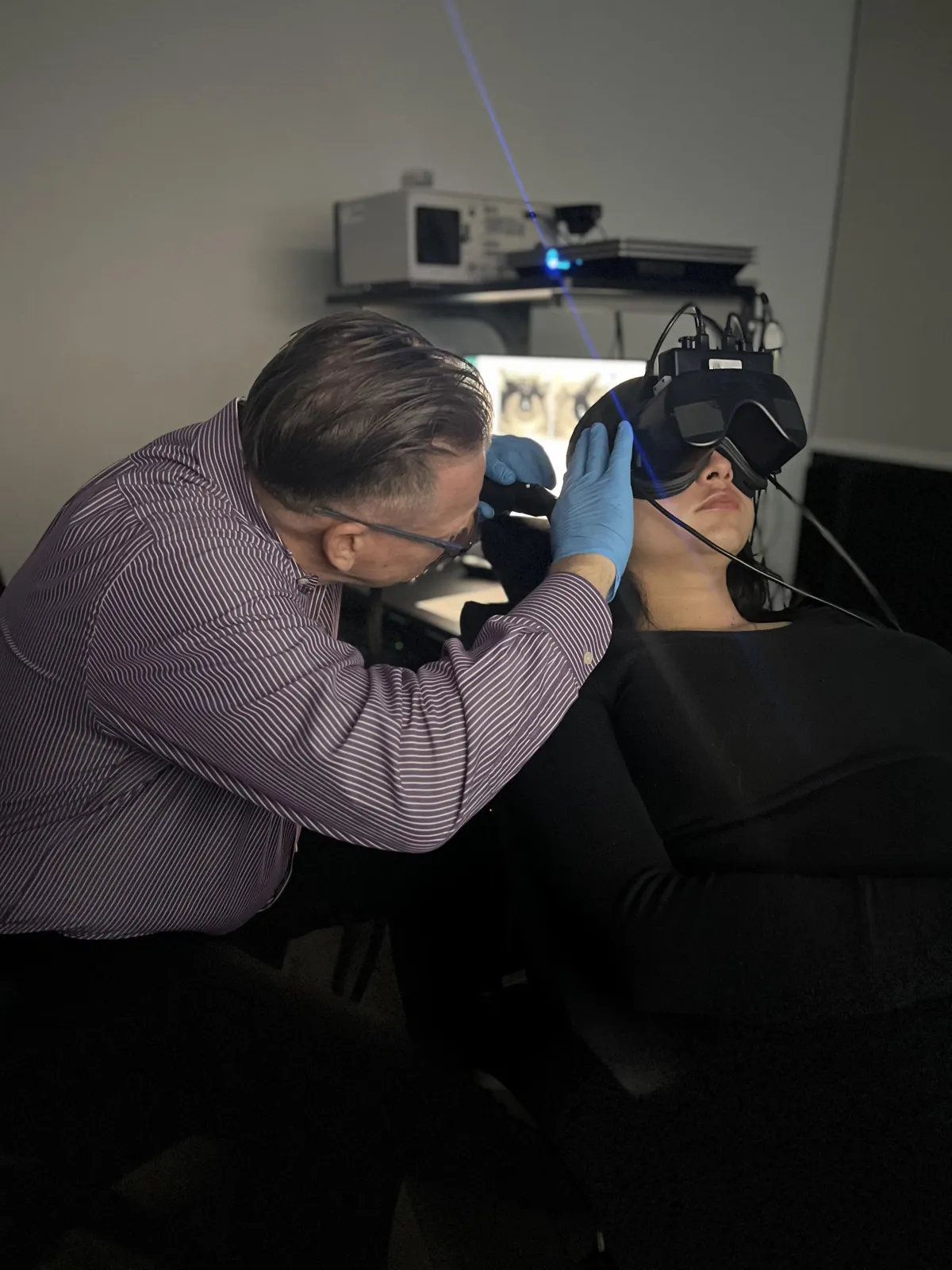
Diagnostic Evaluation
Diagnostic Audiology is not just a Basic 15-minute Hearing Screening
Not all hearing tests are the same. Many retail locations offer basic hearing screenings designed primarily to sell hearing aids. At Doctors of Hearing, we provide comprehensive diagnostic evaluations performed by licensed audiologists to fully understand your hearing health.
The following advanced tests allow our audiologists to determine:
✔ The type and degree of hearing loss
✔ Whether hearing loss may have a medical cause
✔ If a medical referral is needed
✔ The most effective treatment options
Why This Matters
Hearing loss can sometimes be related to medical or neurological conditions. A comprehensive evaluation ensures that important health concerns are not overlooked and that treatment recommendations are accurate, ethical, and personalized.
At Doctors of Hearing, our goal is not simply to sell hearing aids—it is to provide the highest level of diagnostic hearing care and long-term hearing health support.
Comprehensive Hearing Evaluation
This evaluation includes a series of tests that measure your hearing sensitivity, how well you understand speech in quiet and noisy environments, and how well your middle and inner ear are functioning. We also perform a visual examination of the ear and review your medical history to determine if a medical referral may be necessary.

Extensive Patient Case History:
• Prior to testing, the audiologist will collect a detailed case history about the patient. This information helps the audiologist understand possible causes of hearing loss and guides the selection and interpretation of test procedures as well as support additional recommendations for follow-up with other specialists.
• Asking questions regarding hearing concerns
• Inquiring about communication concerns including
• Asking further questions regarding other ear symptoms
• Inquiring about additional medical history including.
Hearing Handicap Inventory for the Elderly (HHIE)
• Assesses the perceived social and emotional impact of hearing loss in older adults
• Uses a self-report questionnaire with 25 questions asking how hearing difficulties affect communication, relationships, and emotional well-being.
• Identifies the degree of perceived hearing handicap, helping audiologists with screening, counseling, and measuring treatment outcomes.
Otoscopic Evaluation:
• Assess the anatomy and structures of the ear canal
• Identify any abnormalities, such as growths, lesions, or tumors
• Examine the tympanic membrane (eardrum) for color, translucency, and position (e.g., retracted, bulging, or normal)
• Detect the presence of cerumen (earwax), fluid, or other foreign material.
It is crucial that the ears are cleared of excessive wax. Otherwise, this can interfere with accurate test results.
WE DO NOT TEST IF EAR CANALS HAVE EXCESSIVE WAX OR THE EAR CANAL IS OCCLUDED WITH WAX.
Tympanometric Testing:
• An objective test assessment of middle ear function and tympanic membrane (eardrum) mobility
• Performed by varying air pressure in the ear canal to measure eardrum response
• Helps evaluate common middle ear concerns such as muffled hearing, tinnitus, ear pressure/fullness, or “popping” sensations
• Abnormal results may indicate the need for medical referral or intervention
• Certain findings can assist in identifying conductive or mixed hearing loss
Acoustic Reflex Testing (Ipsilateral & Contralateral):
• Assesses the function of the middle ear, cochlea, auditory nerve, and brainstem pathways by measuring reflexive contractions of the middle ear muscles in response to sound
• Evaluates the auditory system for potential abnormalities affecting hearing sensitivity or nerve function
• Detects patterns that may help differentiate between sensorineural, conductive, or retrocochlear hearing issues.
Otoacoustic Emissions (OAE) Testing:
• Assesses outer hair cell function in the cochlea by measuring sounds the inner ear produces in response to auditory stimuli.
• Can provide an objective measure of cochlear health in individuals who cannot actively respond to sounds (infants, young children, or certain adults)
• Support diagnostic decisions by helping differentiate between cochlear and retrocochlear hearing problems (e.g., auditory neuropathy, hidden hearing loss, etc.)
Pure Tone Threshold Testing – Air Conduction
• Assesses hearing sensitivity in each ear individually using headphones or inserts
• Determines the softest sounds a person can hear from low to high pitches
• Identifies the degree and configuration of hearing loss (mild, moderate, moderately, severe, severe, or profound)
Pure Tone Threshold Testing – Bone Conduction
• Assesses cochlear (inner ear) hearing sensitivity directly, bypassing the outer and middle ear
• Determines the softest sounds a person can hear from low to high pitches using a bone oscillator placed on the mastoid
• Determines the type of hearing loss (sensorineural, conductive, or mixed) by comparing bone conduction thresholds to air conduction thresholds
• Provides diagnostic information to guide medical or audiologic recommendations
Tone Decay Testing:
• Assesses the ear’s ability to sustain hearing a continuous tone, also referred to as auditory fatigue
• Identifies potential retrocochlear abnormalities, which may indicate issues with the auditory nerve (cranial nerve VIII) or the cerebellopontine angle
• Helps differentiate between cochlear and retrocochlear hearing issues to guide further evaluation or referral
Speech Discrimination Testing:
• Measures the patient’s ability to correctly identify spoken words presented at a comfortable listening level above the hearing threshold
• Provides a percentage score representing how well the patient understands speech in quiet listening conditions
• Sets realistic expectations for hearing aid use, helping patients understand how they may perceive speech with amplification
• Highlights the importance of timely intervention, as delaying hearing aid fitting may reduce future speech understanding
• Supports treatment planning, including hearing aid selection, programming, and auditory rehabilitation strategies
QuickSIN (Speech-in-Noise) Testing
• Assesses the patient’s ability to understand speech in background noise, simulating real-world listening environments
• Sets realistic expectations for communication in noisy environments, guiding counseling and auditory rehabilitation
Most Comfortable Level (MCL) Testing
• Identifies the sound level a patient finds comfortably loud for sustained listening
• Helps guide hearing aid programming and speech testing
• Assesses a patient’s dynamic hearing range by presenting speech or tones while adjusting the intensity up or down in small steps while the patient indicates when the sound feels the most comfortable
Uncomfortable Loudness Level (UCL) Testing
• Identifies sound levels that a patient finds uncomfortably loud
• Helps define a patient’s upper loudness limit to prevent over-amplification
• Assesses a patient’s dynamic hearing range by gradually increasing the intensity of sounds from a comfortable level until the patient signals that the sound has become uncomfortable, before it is painful.
Tinnitus Evaluation
Pitch Matching
• Identifies the pitch (frequency) of the patient’s tinnitus
• The patient listens to tones and selects the closest match
• Results help guide management and sound therapy options
Tinnitus Masking
• Assesses how external sounds affect tinnitus perception
• Narrow band noise is presented at different levels
• Helps determine if sound can reduce or mask the tinnitus
• Findings support treatment recommendations (e.g., sound therapy, hearing aids)
When Should You Schedule
a Comprehensive Hearing Evaluation?
Hearing loss often develops gradually, making it difficult to recognize at first. Many patients do not realize how much they are missing until their hearing is evaluated.
Common signs include:
• Difficulty following conversations in groups
• Trouble hearing in restaurants or crowded environments
• Frequently misunderstanding words
• Avoiding social situations because listening feels exhausting
• Feeling that others speak too softly
• Needing captions when watching television
• Ringing or buzzing in the ears
Addressing hearing concerns early can help prevent communication difficulties, listening fatigue, and social withdrawal.
What Makes Doctors of Hearing Different?
At Doctors of Hearing, we believe hearing care should be thorough, ethical, and patient-centered.
Licensed Audiologists Only: You will always be seen by a licensed audiologist or hearing doctor, never by sales staff or technicians.
Advanced Diagnostic Testing
We provide comprehensive evaluations using state-of-the-art diagnostic equipment to accurately assess hearing, tinnitus, and balance disorders.
Unbiased Hearing Aid Recommendations
We work with the leading hearing aid manufacturers and are not limited to a single brand. This allows us to recommend the best technology for each patient’s needs.
Ethical, Evidence-Based Care
Our team follows professional best practices and clinical guidelines to ensure safe, accurate, and effective treatment.
Personalized Treatment Plans
Every patient is unique. We take the time to understand your hearing needs, lifestyle, and communication goals before recommending solutions.
Schedule Your Comprehensive Hearing Evaluation
If you are experiencing hearing concerns, tinnitus, or balance problems, our audiologists are here to help.
Contact Doctors of Hearing today to schedule your comprehensive evaluation and take the first step toward better hearing.
Try our
Online Hearing Screening
Discover personalized hearing solutions designed to enhance your daily life. Our expert team offers innovative care tailored to meet your unique hearing needs.
Hearing Handicap Inventory for the Elderly (HHIE)
Assesses the perceived social & emotional impact of hearing loss in older adults
Uses a self-report questionnaire with 25 questions asking how hearing difficulties affect communication, relationships, and emotional well-being.
Identifies the degree of perceived hearing handicap, helping audiologists with screening, counseling, and measuring treatment outcomes.
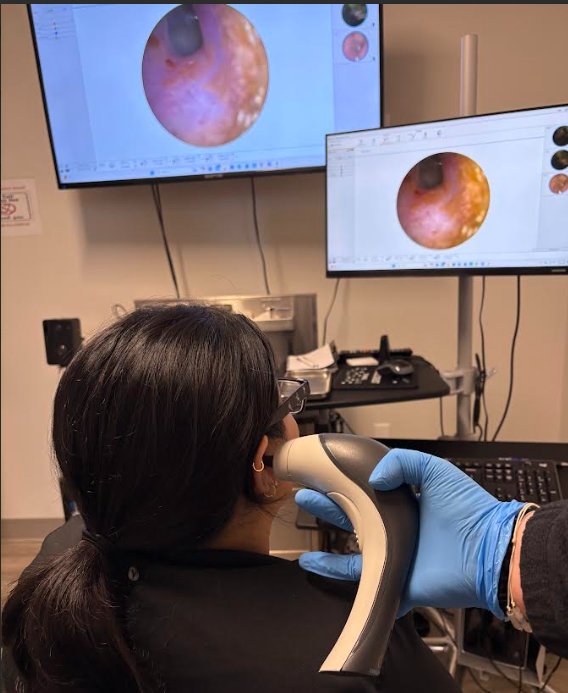
Otoscopic Evaluation:
Assess the anatomy and structures of the ear canal
Identify any abnormalities, such as growths, lesions, or tumors
Examine the tympanic membrane (eardrum) for color, translucency, and position (e.g., retracted, bulging, or normal)
Detect the presence of cerumen (earwax), fluid, or other foreign material
It is crucial that the ears are cleared of excessive wax. Otherwise, this can interfere with accurate test results.
WE DO NOT TEST IF EAR CANALS HAVE EXCESSIVE WAX OR THE EAR CANAL IS OCCLUDED WITH WAX. Audiologist are not able to bill for this service.

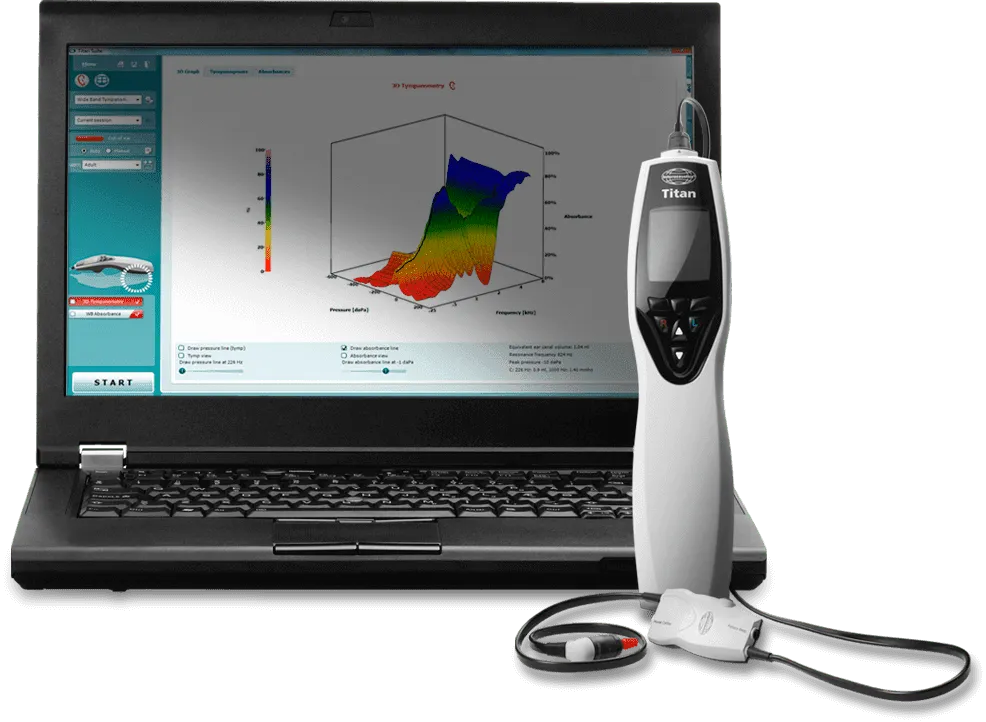
Tympanometric Testing:
An objective test assessment of middle ear function and tympanic membrane (eardrum) mobility
Performed by varying air pressure in the ear canal to measure eardrum response
Helps evaluate common middle ear concerns such as muffled hearing, tinnitus, ear pressure/fullness, or “popping” sensations
Abnormal results may indicate the need for medical referral or intervention
Certain findings can assist in identifying conductive or mixed hearing loss
Acoustic Reflex Testing (Ipsilateral & Contralateral):
Assesses the function of the middle ear, cochlea, auditory nerve, and brainstem pathways by measuring reflexive contractions of the middle ear muscles in response to sound
Evaluates the auditory system for potential abnormalities affecting hearing sensitivity or nerve function
Detects patterns that may help differentiate between sensorineural, conductive, or retrocochlear hearing issues.

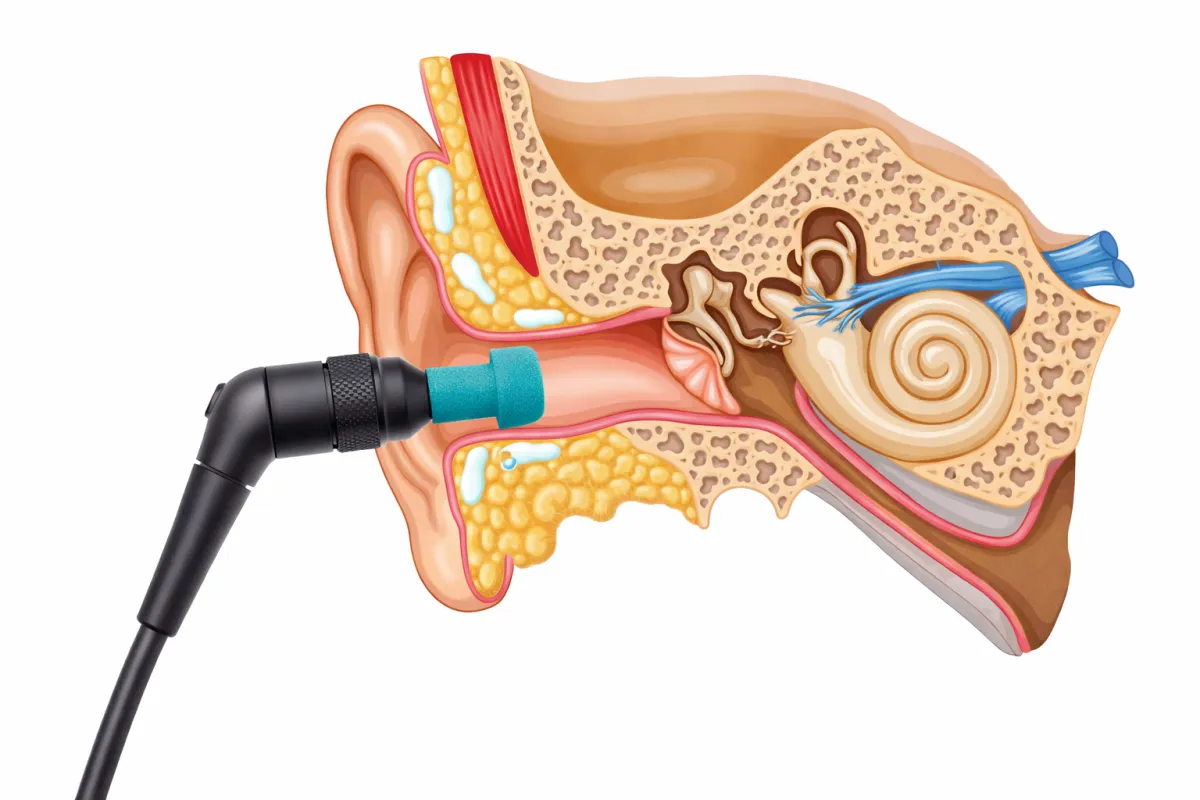
Otoacoustic Emissions (OAE) Testing:
Assesses outer hair cell function in the cochlea by measuring sounds the inner ear produces in response to auditory stimuli
Can provide an objective measure of cochlear health in individuals who cannot actively respond to sounds (infants, young children, or certain adults)
Support diagnostic decisions by helping differentiate between cochlear and retrocochlear hearing problems (e.g., auditory neuropathy, hidden hearing loss, etc.)
Pure Tone Threshold Testing – Air Conduction
Assesses hearing sensitivity in each ear individually using headphones or inserts
Determines the softest sounds a person can hear from low to high pitches
Identifies the degree and configuration of hearing loss (mild, moderate, moderately, severe, severe, or profound)
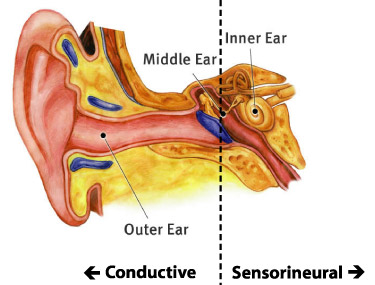
Pure Tone Threshold Testing – Bone Conduction
Assesses cochlear (inner ear) hearing sensitivity directly, bypassing the outer and middle ear
Determines the softest sounds a person can hear from low to high pitches using a bone oscillator placed on the mastoid
Determines the type of hearing loss (sensorineural, conductive, or mixed) by comparing bone conduction thresholds to air conduction thresholds
Provides diagnostic information to guide medical or audiologic recommendations
Tone Decay Testing:
Assesses the ear’s ability to sustain hearing a continuous tone, also referred to as auditory fatigue
Identifies potential retrocochlear abnormalities, which may indicate issues with the auditory nerve (cranial nerve VIII) or the cerebellopontine angle
Helps differentiate between cochlear and retrocochlear hearing issues to guide further
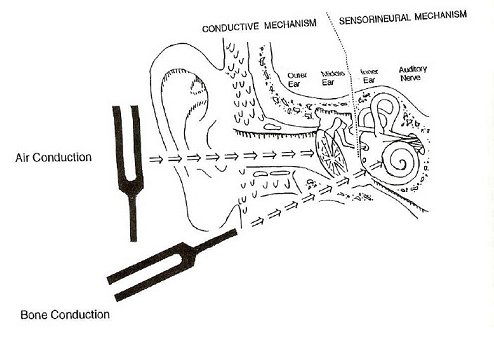

Speech Discrimination Testing:
Measures the patient’s ability to correctly identify spoken words presented at a comfortable listening level above the hearing threshold.
Provides a percentage score representing how well the patient understands speech in quiet listening conditions.
Our testing:
Sets realistic expectations for hearing aid use, helping patients understand how they may perceive speech with amplification
Highlights the importance of timely intervention, as delaying hearing aid fitting may reduce future speech understanding.
Supports treatment planning, including hearing aid selection, programming, and auditory rehabilitation strategies

QuickSIN (Speech-in-Noise) Testing
Assesses the patient’s ability to understand speech in background noise, simulating real-world listening environments
Sets realistic expectations for communication in noisy environments, guiding counseling and auditory rehabilitation
Most Comfortable Level (MCL) Testing
Identifies the sound level a patient finds comfortably loud for sustained listening
Helps guide hearing aid programming and speech testing.
Assesses a patient’s dynamic hearing range by presenting speech or tones while adjusting the intensity up or down in small steps while the patient indicates when the sound feels the most comfortable.
Uncomfortable Loudness Level (UCL) Testing
Identifies sound levels that a patient finds uncomfortably loud
Helps define a patient’s upper loudness limit to prevent over-amplification
Assesses a patient’s dynamic hearing range by gradually increasing the intensity of sounds from a comfortable level until the patient signals that the sound has become uncomfortable, before it is painful

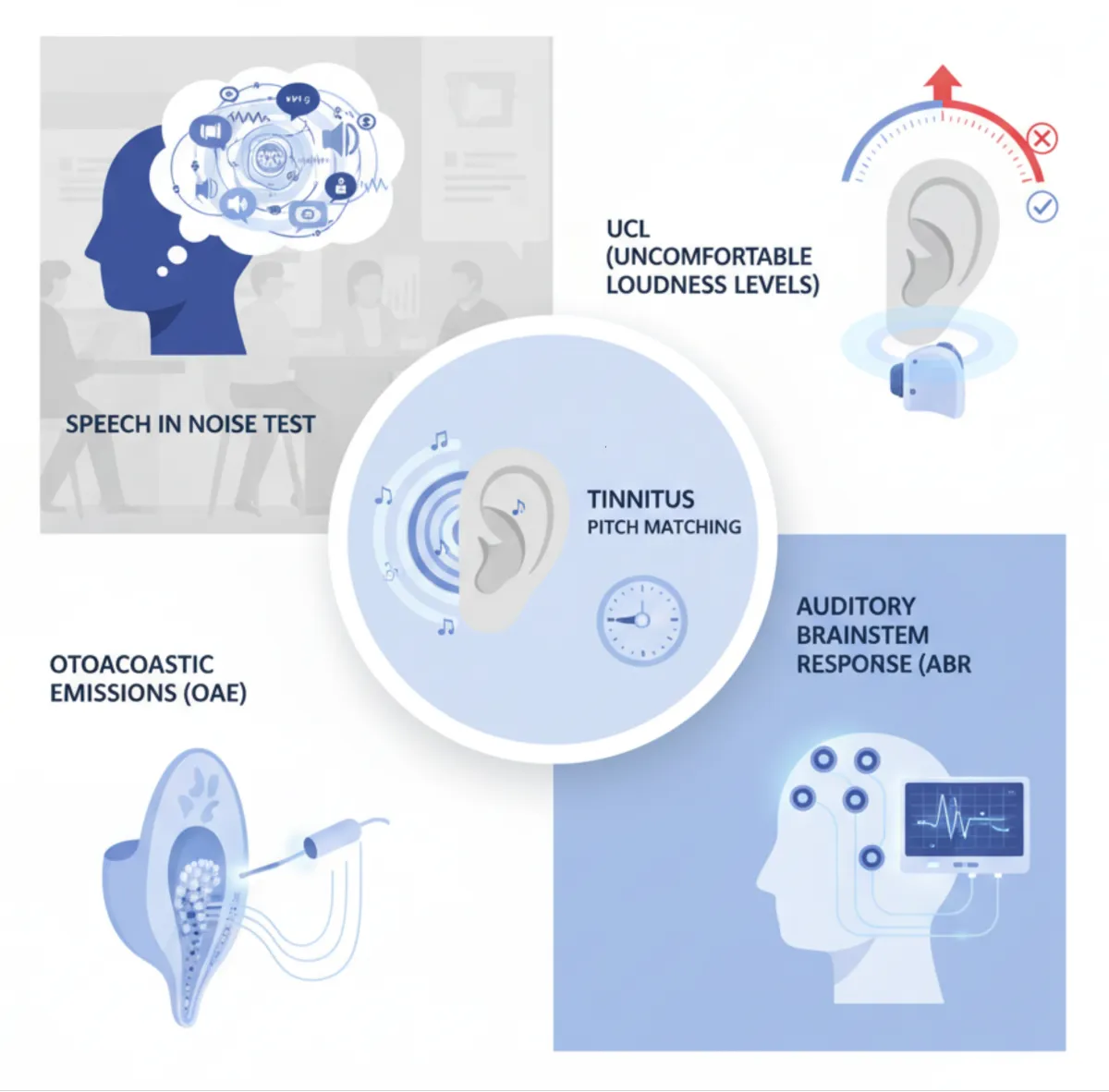
Tinnitus Evaluation
Pitch Matching
Identifies the pitch (frequency) of the patient’s tinnitus
The patient listens to tones and selects the closest match
Results help guide management and sound therapy options
Tinnitus Masking
Assesses how external sounds affect tinnitus perception
Narrow band noise is presented at different levels
Helps determine if sound can reduce or mask the tinnitus
Findings support treatment recommendations (e.g., sound therapy, hearing aids)

Videonystagmography (VNG): Involves the use of infrared goggles to track eye movements during visual stimulation and positional changes. VNG can determine whether dizziness is caused by inner ear disease as opposed to a central nervous system pathology.
When a patient comes to an Audiologist office, our main concern is: is there anything medical going on in the ears that can be medically treated prior to use of hearing aids? Yes, we want to help people hear better and hence the recommendation of hearing aids but we are also concern about the medical aspect of our patients.
We offer all of the above tests in our Pasadena office and in our Rancho Cucamonga office as well but we also offer ABR and Vestibular testing in our Rancho Cucamonga office. If a patient needs an ABR or vestibular testing, they can visit our Rancho Office.